| Vascular disease | |
|---|---|
 | |
| Veins and arteries | |
| Specialty | Angiology |
| Types | Peripheral artery disease,[1] Renal artery stenosis[2] |
| Diagnostic method | Venography, Ultrasound[3] |
| Treatment | Quit smoking, Lower cholesterol[4] |
Vascular disease is a class of diseases of the vessels of the circulatory system in the body, including blood vessels – the arteries and veins, and the lymphatic vessels. Vascular disease is a subgroup of cardiovascular disease. Disorders in this vast network of blood and lymph vessels can cause a range of health problems that can sometimes become severe, and fatal.[3] Coronary heart disease for example, is the leading cause of death for men and women in the United States.[5]
Types
There are several types of vascular disease, including venous diseases, and arterial diseases, and signs and symptoms vary depending on the disease. Those of the arterial system are associated with blood supply to tissues and its obstruction due to blockages or narrowing. In the venous system disorders are often caused by a slow return of blood due to insufficient valves, or to a blood clot.[6]
Venous disease
Most disorders of the veins involve obstruction such as a thrombus or insufficiency of the valves, or both of these.[7][8][9] Other conditions may be due to inflammation.
Phlebitis
Phlebitis is the inflammation of a vein. It is usually accompanied by a blood clot when it is known as thrombophlebitis. When the affected vein is a superficial vein in the leg, it is known as superficial thrombophlebitis, and unlike deep vein thrombosis there is little risk of the clot breaking off as an embolus.[10]
Venous insufficiency
Venous insufficiency is the most common disorder of the venous system, and is usually manifested as either spider veins or varicose veins. Several treatments are available including endovenous thermal ablation (using radiofrequency or laser energy), vein stripping, ambulatory phlebectomy, foam sclerotherapy, laser, or compression.
Postphlebitic syndrome is venous insufficiency that develops following deep vein thrombosis.[11]
Venous thrombosis
Venous thrombosis is the formation of a thrombus (blood clot) in a vein. This most commonly affects a deep vein known as deep vein thrombosis (DVT). DVT usually occurs in the veins of the legs, although it can also occur in the veins of the arms. Immobility, active cancer, obesity, traumatic damage and congenital disorders that make clots more likely are all risk factors for deep vein thrombosis. It can cause the affected limb to swell, and cause pain and an overlying skin rash. In the worst case, a deep vein thrombosis can extend, or a part of a clot can break off as an embolus and lodge in a pulmonary artery in the lungs, known as a pulmonary embolism.The decision to treat deep vein thrombosis depends on its size, a person's symptoms, and their risk factors. It generally involves anticoagulation to prevents clots or to reduce the size of the clot. Intermittent pneumatic compression is a method used to improve venous circulation in cases of edema or in those at risk from a deep vein thrombosis.
A clot can also form in a superficial vein (superficial venous thrombosis) which is normally not clinically significant, but the thrombus can migrate into the deep venous system where it can also give rise to a pulmonary embolism.[12]
Portal hypertension
The portal vein also known as the hepatic portal vein carries blood drained from most of the gastrointestinal tract to the liver. Portal hypertension is mainly caused by cirrhosis of the liver. Other causes can include an obstructing clot in a hepatic vein (Budd Chiari syndrome) or compression from tumors or tuberculosis lesions. When the pressure increases in the portal vein, a collateral circulation develops, causing visible veins such as esophageal varices.
Vascular anomalies
A vascular anomaly can be either a vascular tumor or a birthmark, or a vascular malformation. [13] In a tumor such as infantile hemangioma the mass is soft, and easily compressed, and their coloring is due to the dilated anomalous involved veins.[14] They are most commonly found in the head and neck. Venous malformations are the type of vascular malformation that involves the veins. They can often extend deeper from their surface appearance, reaching underlying muscle or bone.[15] In the neck they may extend into the lining of the mouth cavity or into the salivary glands.[14] They are the most common of the vascular malformations.[16] A severe venous malformation can involve the lymph vessels as a lymphaticovenous malformation.[14]
Arterial disease
- Coronary artery disease – the most common of the cardiovascular diseases, types include angina, and myocardial infarction
- Carotid artery stenosis – any narrowing of the carotid arteries
- Peripheral artery disease – occurs when atheromatous plaques build up in the arteries that supply blood to the arms and legs, causing the arteries to narrow or become blocked.[1]
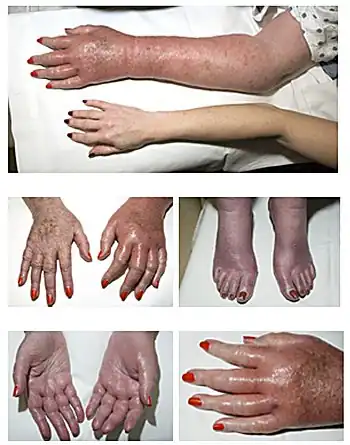
- Erythromelalgia - a rare peripheral vascular disease with symptoms that include burning pain, increased temperature, erythema and swelling that generally affect the hands and feet. [17]
- Renal artery stenosis - the narrowing of renal arteries that carry blood to the kidneys from the aorta.[2]
- Buerger's disease – inflammation and swelling in small blood vessels, causing the vessels to narrow or become blocked by blood clots.[18]
- Raynaud syndrome – a peripheral vascular disorder that causes constriction of the peripheral blood vessels in the fingers and toes when a person is cold or experiencing stress.[19]
- Disseminated intravascular coagulation – a widespread activation of clotting in the smaller blood vessels.[20]
- Cerebrovascular disease – a group of vascular diseases that affect brain function, most commonly a stroke.[21]
- Vasculitis - inflammation of blood vessels, either arteries or veins
Lymphatic disease
Mechanism

Vascular disease is a pathological state of large and medium muscular arteries and is triggered by endothelial cell dysfunction.[22]
Because of factors like pathogens, oxidized LDL particles and other inflammatory stimuli endothelial cells become active.[23]
The process causes thickening of the vessel wall, forming a plaque that consists of proliferating smooth muscle cells, macrophages and lymphocytes.[24][25]
The plaque results in restricted blood flow, decreasing the amount of oxygen and nutrients that reach certain organs.[26]
This plaque can also rupture, causing the formation of clots.[27]
Diagnosis
Diagnosing vascular disease can be complex due to the variety of symptoms vascular diseases can cause. Reviewing a patient's family history and conducting a physical examination are important steps in making a diagnosis. Physical exams may differ depending on the type of vascular disease suspected. For example, in the case of a peripheral vascular disease, a physical exam consists of checking blood flow in a patient's legs.[28][29]
Treatment

Treatment varies based on the type of vascular disease being treated. In treating renal artery disease, a 2014 study indicates that balloon angioplasty can improve diastolic blood pressure and potentially reduce antihypertensive drug requirements.[30] In the case of peripheral artery disease, treatment to prevent complications is important; without treatment, sores or gangrene (tissue death) may occur.
More generally, treatments for vascular disease may include:[4]
- Lowering cholesterol levels
- Lowering blood pressure
- Lowering blood glucose
- Changes in diet
- Increasing physical activity (as recommended by a healthcare provider)
- Weight loss
- Quitting smoking
- Stress reduction
References
- 1 2 "Peripheral Arterial Disease: MedlinePlus". www.nlm.nih.gov. Retrieved 2015-06-23.
- 1 2 "Renal Artery Stenosis". www.niddk.nih.gov. Retrieved 2015-06-23.
- 1 2 "Vascular Diseases: MedlinePlus". www.nlm.nih.gov. Retrieved 2015-06-23.
- 1 2 "How Is Peripheral Arterial Disease Treated? - NHLBI, NIH". www.nhlbi.nih.gov. Retrieved 2015-06-23.
- ↑ "Coronary Artery Disease". medlineplus.gov. Retrieved 13 February 2023.
- ↑ Hirsch, Alan T.; Haskal, Ziv J.; Hertzer, Norman R.; Bakal, Curtis W.; Creager, Mark A.; Halperin, Jonathan L.; Hiratzka, Loren F.; Murphy, William R.C.; Olin, Jeffrey W.; Puschett, Jules B.; Rosenfield, Kenneth A.; Sacks, David; Stanley, James C.; Taylor, Lloyd M.; White, Christopher J.; White, John; White, Rodney A.; Antman, Elliott M.; Smith, Sidney C.; Adams, Cynthia D.; Anderson, Jeffrey L.; Faxon, David P.; Fuster, Valentin; Gibbons, Raymond J.; Halperin, Jonathan L.; Hiratzka, Loren F.; Hunt, Sharon A.; Jacobs, Alice K.; Nishimura, Rick; et al. (2006). "ACC/AHA 2005 Guidelines for the Management of Patients With Peripheral Arterial Disease (Lower Extremity, Renal, Mesenteric, and Abdominal Aortic): A Collaborative Report from the American Association for Vascular Surgery/Society for Vascular Surgery,⁎ Society for Cardiovascular Angiography and Interventions, Society for Vascular Medicine and Biology, Society of Interventional Radiology, and the ACC/AHA Task Force on Practice Guidelines (Writing Committee to Develop Guidelines for the Management of Patients With Peripheral Arterial Disease)". Journal of the American College of Cardiology. 47 (6): e1–e192. doi:10.1016/j.jacc.2006.02.024. Retrieved 2016-02-02.
- ↑ Goel, RR; Hardy, SC; Brown, T (30 September 2021). "Surgery for deep venous insufficiency". The Cochrane Database of Systematic Reviews. 2021 (9): CD001097. doi:10.1002/14651858.CD001097.pub4. PMC 8483065. PMID 34591328.
- ↑ Publishing, Licorn (9 April 2013). "The venous valves of the lower limbs". Servier - Phlebolymphology. Retrieved 9 January 2023.
- ↑ "20.1 Structure and Function of Blood Vessels - Anatomy and Physiology 2e | OpenStax". openstax.org. Retrieved 25 January 2023.
- ↑ Di Nisio M, Wichers IM, Middeldorp S (February 2018). "Treatment for superficial thrombophlebitis of the leg". Cochrane Database Syst Rev. 2018 (2): CD004982. doi:10.1002/14651858.CD004982.pub6. PMC 6953389. PMID 29478266.
- ↑ Kahn SR (August 2006). "The post-thrombotic syndrome: progress and pitfalls". British Journal of Haematology. 134 (4): 357–65. doi:10.1111/j.1365-2141.2006.06200.x. PMID 16822286. S2CID 19715556.
- ↑ Cosmi, B. (July 2015). "Management of superficial vein thrombosis". Journal of Thrombosis and Haemostasis. 13 (7): 1175–1183. doi:10.1111/jth.12986. PMID 25903684.
- ↑ Steiner, JE; Drolet, BA (September 2017). "Classification of Vascular Anomalies: An Update". Seminars in Interventional Radiology. 34 (3): 225–232. doi:10.1055/s-0037-1604295. PMC 5615389. PMID 28955111.
- 1 2 3 Chim, H; Drolet, B; Duffy, K; Koshima, I; Gosain, AK (August 2010). "Vascular anomalies and lymphedema". Plastic and Reconstructive Surgery. 126 (2): 55e–69e. doi:10.1097/PRS.0b013e3181df803d. PMID 20679788. S2CID 30865392.
- ↑ Chen, RJ; Vrazas, JI; Penington, AJ (January 2021). "Surgical Management of Intramuscular Venous Malformations". Journal of Pediatric Orthopedics. 41 (1): e67–e73. doi:10.1097/BPO.0000000000001667. PMID 32815867. S2CID 221199574.
- ↑ Markovic, JN; Shortell, CK (October 2021). "Venous malformations". The Journal of Cardiovascular Surgery. 62 (5): 456–466. doi:10.23736/S0021-9509.21.11911-1. PMID 34105926.
- ↑ "Erythromelalgia". nhs.uk. 2017-10-18. Retrieved 2019-01-04.
- ↑ "Thromboangiitis obliterans: MedlinePlus Medical Encyclopedia". www.nlm.nih.gov. Retrieved 2015-06-23.
- ↑ "Raynaud's Disease: MedlinePlus". www.nlm.nih.gov. Retrieved 2015-06-23.
- ↑ "Disseminated intravascular coagulation (DIC): MedlinePlus Medical Encyclopedia". www.nlm.nih.gov. Retrieved 2015-06-25.
- ↑ "Stroke". nhs.uk. 2017-10-24. Retrieved 2022-06-29.
- ↑ Rajendran, Peramaiyan; Rengarajan, Thamaraiselvan; Thangavel, Jayakumar; Nishigaki, Yutaka; Sakthisekaran, Dhanapal; Sethi, Gautam; Nishigaki, Ikuo (2013). "The Vascular Endothelium and Human Diseases". International Journal of Biological Sciences. 9 (10): 1057–1069. doi:10.7150/ijbs.7502. ISSN 1449-2288. PMC 3831119. PMID 24250251.
- ↑ Bikfalvi, Andreas (2013-12-19). Encyclopedic Reference of Vascular Biology & Pathology. Springer. ISBN 9783642570636.
- ↑ Rubin, Emanuel; Damjanov, Ivan (2013-11-11). Pathology Reviews · 1989. Springer Science & Business Media. ISBN 9781461245025.
- ↑ Gunstone, Frank D.; Harwood, John L.; Dijkstra, Albert J. (2007-03-13). The Lipid Handbook with CD-ROM, Third Edition. CRC Press. ISBN 9781420009675.
- ↑ Rolfes, Sharon Rady; Pinna, Kathryn; Whitney, Ellie (2011-06-20). Understanding Normal and Clinical Nutrition. Cengage Learning. ISBN 978-0840068453.
- ↑ Ząbczyk, Michał; Natorska, Joanna; Undas, Anetta (2021-07-05). "Fibrin Clot Properties in Atherosclerotic Vascular Disease: From Pathophysiology to Clinical Outcomes". Journal of Clinical Medicine. 10 (13): 2999. doi:10.3390/jcm10132999. ISSN 2077-0383. PMC 8268932. PMID 34279484.
- ↑ "How Is Peripheral Arterial Disease Diagnosed? - NHLBI, NIH". www.nhlbi.nih.gov. Retrieved 2015-06-23.
- ↑ Andras, Alina; Ferket, Bart (2014). "Screening for peripheral arterial disease". Cochrane Database of Systematic Reviews (4): CD010835. doi:10.1002/14651858.CD010835.pub2. PMID 24711093.
- ↑ Jenks, Sara; Yeoh, Su Ern; Conway, Bryan R. (2014). "Balloon angioplasty, with and without stenting, versus medical therapy for hypertensive patients with renal artery stenosis". The Cochrane Database of Systematic Reviews. 12 (12): CD002944. doi:10.1002/14651858.CD002944.pub2. ISSN 1469-493X. PMC 7138037. PMID 25478936.
Further reading
- "The effects of lowering LDL cholesterol with statin therapy in people at low risk of vascular disease: meta-analysis of individual data from 27 randomised trials". www.crd.york.ac.uk. Retrieved 2015-06-23.